by Gaurav Dubey (MS Biotechnology)
Co-Founder & President, Karmik, LLC
Illicit opioid abuse is the single most pressing substance abuse problem in the United States and throughout the world.1 Opioids are a class of narcotic, pain-relieving drugs that include hydrocodone (Vicodin), oxycodone (Percocet), Oxycontin, morphine, heroin, and fentanyl, among others. Over the last decade, the United States and the world at large have witnessed increasing numbers of individuals becoming severely addicted to opiates. Behavioral interventions alone have shown poor outcomes, with over 80% of patients returning to active drug use.1 As a result, it has become of paramount importance to determine efficacious pharmacologic treatments that can adequately supplement behavioral therapy in rehabilitating patients suffering from addiction. In this article, we will be accessing the controversy of Buprenorphine Treatment For Opioid Addiction.
Studies Show Medication-Assisted Treatment Is Efficacious In Treating Opioid Use Disorder
Studies have shown that adjunctive medication-assisted treatment (MAT) therapy, along with adequate behavioral interventions, provides the best opportunity for patients to achieve a long-lasting, successful recovery from opiate addiction. The three pharmacologic agents used in MAT therapy are methadone, buprenorphine, and extended-release naltrexone (also known as Vivitrol). This blog will explore buprenorphine (sometimes referred to colloquially as “bupe”) maintenance therapy, its clinical utility in treating opioid addiction, and various risks that are worth noting when considering this treatment modality.2

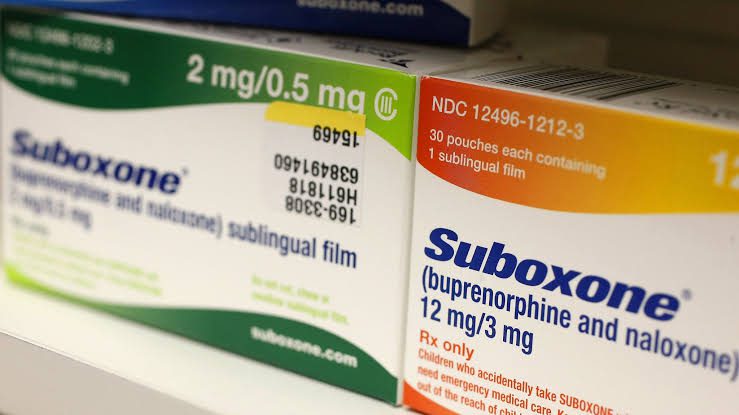
Suboxone: The Most Commonly Used Formulation of Buprenorphine for MAT
As discussed in our evidence-based review of methadone, using pharmacologically active opioids to treat opioid addiction has long been a cornerstone of medical rehabilitation for opioid addicts. Until recently, methadone has always been considered the “gold standard” in MAT therapy. However, the development of Suboxone (a combination of buprenorphine and naloxone in a 4:1 ratio) presents some novel advantages, leading healthcare practitioners to favor this treatment modality. Suboxone is currently the most common form of buprenorphine used for MAT today.

The Addition of the Opioid Overdose “Antidote” Naloxone Is Said To Deter Abuse

The addition of naloxone, an opioid antagonist used to reverse opioid overdose, is supposedly added to the formulation in order to deter intravenous abuse.* The advent of Suboxone to treat opioid addiction was considered a medical advancement beyond that of methadone; however, both drugs present novel advantages and disadvantages. Recent studies show that buprenorphine (Suboxone) is equivalent in efficacy to that of methadone when “sufficient buprenorphine doses, rapid induction, and flexible dosing are used.”3 To better understand and characterize the role of Suboxone in opioid addiction and recovery, it is necessary to gain a better understanding of its basic pharmacology.
Basic Buprenorphine Pharmacology in the Treatment of Opioid Addiction
Buprenorphine is a partial opioid agonist and antagonist drug that exhibits a unique pharmacology. Unlike traditional full-agonist drugs like heroin, buprenorphine is a partial agonist at the μ-opioid receptor, where it displays a significantly lower intrinsic activity.4 That is to say, buprenorphine causes less euphoria, sedation, and analgesia than methadone, but it is nonetheless still able to attenuate withdrawal symptoms.4 This pharmacological property of buprenorphine alone allows it to confer major advantages over methadone for use as an opioid replacement therapy. Most notably, Suboxone has significantly lower abuse potential than methadone. **
Buprenorphine’s Extra-Long Half-Life Allows for 72-Hour Dosing Intervals
“The slow association/dissociation kinetics allow for 72-hour dosing intervals in buprenorphine treatment.”5 This presents a unique advantage over methadone, which requires daily dosing. In addition to there being no need to attend a clinic daily, multiple-day dosing intervals allow the patient greater freedom. However, this also inevitably means that greater quantities of drugs like Suboxone will be available for diversion, ending up in the illicit trade.
There’s An Argument To Be Made for Buprenorphine Accessibility, But It’s Not Without Its Risks

Nevertheless, due to the safety profile of Suboxone and the fact that many users try to procure it on the black market in order to treat withdrawals or for harm reduction purposes, there is an argument to be made for making it easily accessible. However, buprenorphine is still an addictive narcotic, and its abuse potential and addiction liability should be carefully taken into account when considering policy decisions. Studies have found that “illicit buprenorphine use is correlated with better treatment outcomes in primary care buprenorphine programs.”6 Indeed, this research found that the typical illicit bupe user seems to have financial constraints and is attempting to practice harm reduction.6
Analysis Suggests Increased Access Will Reduce Illicit Bupe Diversion
A recent social network analysis of buprenorphine diversion discovered that “increasing access to providers reduced diversion rates” of buprenorphine.7 Thus, the argument for better access to Suboxone as a tool for harm reduction should not be easily dismissed and should be further analyzed in an evidence-based context to better shape drug policy.
Buprenorphine’s “Ceiling Effect” & Blocking Effect Reduces Overdose & Relapse Risk
Another key reason for considering increasing the accessibility of buprenorphine is its “ceiling effect,” which prevents overdose risk by negating additional reinforcing or agonistic effects after a certain point, despite increasing dosage. Finally, out of all the drugs that are known to act upon the μ-opioid receptor, buprenorphine has one of the strongest binding affinities. As such, it is incredibly difficult to “displace” buprenorphine that is attached to the opioid receptors. Therefore, buprenorphine/Suboxone maintenance effectively “blocks” the effects of illicit opioid use, deterring relapse. This is accomplished in a somewhat similar fashion as high-dose methadone, which can produce a blocking effect to deter relapse, as well. Vivitrol, the extended-release naltrexone injection, also produces a “blockade effect” but is also non-habit forming, non-narcotic, and thus, non-addictive. To learn more about Vivitrol as a tool in treating opioid addiction, check out our evidence-based review of Vivitrol here.

Buprenorphine Assisted Therapy: Simply Trading One Addiction For Another?
Many people view buprenorphine/Suboxone, along with methadone MAT treatment, as simply “trading one addiction for another.” Indeed, drugs like methadone and suboxone do occupy the same brain receptor as drugs like heroin, but to end their comparison there is a severe oversimplification of the full pharmacologic profile of MAT drugs compared to drugs of abuse.
Distinct Pharmacological Differences Between Long-Acting MAT Drugs & Short-Acting Opioids of Abuse
Studies have shown that there are distinct “pharmacological differences between long-acting opiate (L-AO) medications (like methadone and Suboxone) and short-acting opioids (like heroin) in terms of reinforcing properties, pharmacokinetics, and effects on the endocrine and immune systems.”8 Due to their unique pharmacological profile, “L-AOs contribute to control addictive behavior, reduce craving, and restore the balance of disrupted endocrine function.”8
Viewing MAT Patients As Active Addicts Is a Damaging Misconception

Since L-AO therapy helps individuals lead healthier lives and begin the process of recovery, it is a damaging misunderstanding to view an addict engaging in MAT— under the care of a medical professional—as simply trading one addiction for another. Indeed, MAT, combined with behavioral intervention, has been shown to markedly improve the quality of life and help rehabilitate addicts.1
Is Long-Term MAT Therapy Right For Me?
While many ultimately do choose to detox off long-term MAT pharmacotherapy and live free of chemical dependency, in other cases, it may benefit the patient to be maintained on MAT for long periods of time. This is especially true for patients with severe chronic pain. For these patients, drugs like Suboxone may be a more suitable, practical, and safer option than methadone, saving them from a daily drive to a clinic, and offering treatment with a generally reduced risk of overdose. If you or someone you know is struggling with opioid addiction or is interested in successfully detoxing off methadone, contact us at EvolveIndy.com to learn more about medically supervised, clinical methadone and Suboxone detox.
For The Many That Desire To Be Free: A Word About Suboxone Withdrawal
However, for many, the side effect profile of methadone and buprenorphine, or simply the desire to be free of dependency after years of drug use, lead them to ultimately taper and discontinue treatment. Withdrawal from long-acting opioid drugs like methadone and Suboxone is often very long and protracted (on the order of weeks), compared to withdrawal from short-acting opioids like heroin, which has much shorter half-lives and elimination times (with acute withdrawal generally only lasting several days).
Suboxone Withdrawal May Be Milder, But It’s Much Longer Than Traditional Opiate Withdrawal and Makes Detoxing Difficult For Many
Withdrawal from long-term Suboxone use is reported in the clinical literature as “milder” than the acute withdrawal that ensues from drugs like heroin. Nonetheless, it is firmly established in anecdotal reports that this “milder but significantly longer” period of withdrawal is far more difficult to endure than traditional opiate withdrawal. As such, withdrawal from drugs like Suboxone and methadone is best conducted at detox facilities while under the guidance of well-trained medical professionals. To learn more about how you can seek professional help to detox from methadone and Suboxone, visit EvolveIndy.com.
A Cautionary Note About Precipitated Withdrawal From Buprenorphine
Buprenorphine’s incredibly high affinity for the μ-opioid receptor means that it will “displace any existing circulating opioids.”4 This presents a challenging and novel clinical problem when initiating buprenorphine/Suboxone therapy for opioid addiction: the phenomenon of precipitated withdrawal.4 In English, this translates to buprenorphine (a partial-agonist that does not stimulate the μ-opioid receptor as much as full-agonist drugs) effectively “kicking out” any drugs occupying the opioid receptor and thereafter taking their place. If a patient is dependent on full-agonist drugs, such as heroin, buprenorphine administration will result in the rapid onset of intense withdrawal symptoms, such as cold sweats, diarrhea, cramping, anxiety, panic attacks, and dilated pupils.9
Great caution must be exercised when introducing heroin users to buprenorphine treatment, and an adequate COWS score (the “clinical opiate withdrawal scale” that assesses the level of opioid withdrawal currently being experienced) should be reached before buprenorphine administration.10 The COWS scale is an 11-item clinician-administered scale assessing opioid withdrawal.10 Once enough of the full-acting opioid agonist has left the patient’s body (usually 24 hours of abstinence from heroin use is recommended to safely transition), buprenorphine maintenance therapy can safely begin.

Transitioning to Buprenorphine From Methadone Is Incredibly Challenging
The risk of precipitated withdrawal is greatly magnified when attempting to switch from methadone to buprenorphine. This is due to the long half-life of the full-agonist drug, methadone. A 2004 study by McNicholas demonstrated that patients above 30mg of methadone should not receive buprenorphine therapy.11 Unlike traditional short-acting opioids, one must abstain from methadone use for up to one week before being able to be inducted into buprenorphine treatment. For anyone familiar with opioid dependence, going seven days without a methadone dose after being a daily patient (oftentimes for years) is a daunting task.
The Bernese Method: A Novel Approach for Co-Administration of Micro-dosed Buprenorphine With Overlapping Full-Agonist Opioid Use
Due to the risk of relapse from tapering full-agonist illicit opioid use to effectively induct buprenorphine therapy, a novel method has been proposed for the concurrent administration of buprenorphine with full-agonist opioids. Termed the Bernese Method, this protocol involves micro-dosing buprenorphine at the same time that one is still dosing full-agonist opioids. When done at low enough doses, one is able to avoid incredibly unpleasant withdrawal symptoms. A 1997 paper even showed a 0.2mg IV dose of buprenorphine in methadone-maintained patients did not precipitate withdrawal.12

Side Effects & Adverse Events Relating to Buprenorphine
Several side effects have been associated with buprenorphine treatment. The most common side effects of buprenorphine are:
- Headache
- Anxiety
- Insomnia
- Sweating
- Constipation
- Nausea
- Opioid Withdrawal Symptoms upon Cessation
Contact your doctor or healthcare provider immediately if you notice any of the following symptoms:
- Fainting
- Fast or Irregular Heartbeat
- Severe Dizziness
- Shallow or Depressed Breathing
- Unusual Drowsiness or Difficulty Waking up
Managing side effects from MAT drugs like methadone and Suboxone can be quite challenging for many users. In particular, there is a great deal of clinical evidence stating that severe constipation caused by these drugs can seriously interfere with and detract from one’s quality of life. Indeed, as witnessed by recent super bowl commercials, opioid-induced constipation (OIC) drugs are best-sellers right now, perhaps standing as a chilling testament to just how prevalent the opioid epidemic has become.
How Long Should Buprenorphine Be Used For In Opioid Detoxification?
While many protocols and studies advocate for the long-term use of buprenorphine for full-agonist opioid detoxification and relapse prevention, “one guideline suggests that a daily dose of Suboxone for 1 to 3 days should eliminate signs and symptoms of opioid withdrawal, suppress opioid cravings, and eliminate illicit opioid use in adults”.13 The benefit of buprenorphine cessation after overcoming acute opioid withdrawal is the opportunity for antagonist therapy (e.g. Vivitrol injection), which can be used for long-term maintenance without the development of dependence.
To learn more about Vivitrol, check out our evidence-based review of Vivitrol here.
Closing Thoughts on the Safety & Efficacy of Buprenorphine Treatment for Opioid Addiction
Increasingly, the clinical community is considering buprenorphine treatment an “attractive” and “underutilized” approach. Amidst the desolation of the current opioid epidemic, the need for any and all effective treatments is at an all-time high. Buprenorphine-containing drugs like Suboxone play a novel role in combating the opioid epidemic, particularly due to their immense safety profile—especially when compared to the predecessor, methadone. Are increased Suboxone prescriptions actually helping quell this epidemic? It’s hard to provide a categorically definite answer. While some studies have certainly proven bupe’s efficacy, other recent findings draw this conclusion into question. For instance, “Suboxone is apparently now the No. 1 prescribed drug in Tennessee, but in spite of this overdose death rates have gone up in Tennessee, so there is no evidence that rising Suboxone prescriptions have decreased overdose deaths [in Tennessee].”14
As research continues to discover better treatment modalities for opioid use disorder, further study into buprenorphine as a key agent in the battle against opioid addiction is vital. It is imperative to better study and characterizes whether buprenorphine maintenance therapy can be efficacious at eliminating withdrawal and successfully helping opioid-dependent users on their path to recovery, and highly recommended by this biologist and author in recovery.

*Footnote #1: The addition of naloxone to Suboxone is purportedly to deter IV abuse of the drug. Manufacturers of Suboxone claim that although naloxone has poor bioavailability sublingually (how the medication is supposed to be taken), it can precipitate withdrawal and/or block the effects of buprenorphine if Suboxone is injected.15 However, clinical literature suggests buprenorphine has one of the highest affinities for the μ-opioid receptor, even beyond that of naloxone. As such, it wouldn’t make sense for the naloxone to “displace” buprenorphine when competing for the receptor site, even if the drug were injected. If one is already dependent on full-agonist opiates, consuming Suboxone at even the lowest recommended dosages for addiction maintenance would result in precipitated withdrawal syndrome, which is extremely uncomfortable and potentially dangerous. However, this syndrome is the result of buprenorphine (a partial opioid agonist) displacing full-agonist opioids such as oxycodone, morphine, or heroin. Using Suboxone, even intravenously, when already on Suboxone for MAT therapy does not precipitate withdrawal since the naloxone is essentially pharmacologically “inert” compared to the buprenorphine. In fact, at least 3 studies have demonstrated that “at least some individuals may not experience precipitated withdrawal when injecting the BPN/NLX co-formulation.16–18Even worse, another study found that even in patients who did report withdrawal from injecting Suboxone, this did not result in a decrease in the self-administered BPN/NLX dose.19
There is some anecdotal evidence that the naloxone present in Suboxone may cause side-effects (mainly headaches) that can be avoided by prescribing patients Subutex (a pure buprenorphine hydrochloride formulation), instead.
There is also some speculation that the real reason naloxone was added to buprenoprhine when creating Suboxone was so that a novel patent could be secured for what was certain to become a blockbuster drug (since Subutex, a buprenorphine-only drug, was already on the market). Of course, since Suboxone was intended to treat substance abusers, touting the “anti-abuse” mechanism offered by the addition of naloxone was a huge-selling point for the drug. It is worth mentioning that the manufacturers of Suboxone, Reckitt Benckiser Group (RB Group) is currently wrapped up in an incredibly large criminal and civil fraud investigation into the marketing of Suboxone.20 “The resolution – the largest recovery by the United States in a case concerning an opioid drug – includes the forfeiture of proceeds totaling $647 million, civil settlements with the federal government and the states totaling $700 million, and an administrative resolution with the Federal Trade Commission for $50 million.”20
** Footnote #2:The pharmacological mechanism of buprenorphine is incredibly unique and expresses completely different properties at different doses. Buprenorphine, the active compound in drugs like Suboxone, is known to have a biphasic dose-response curve. At low microgram doses, buprenorphine is metabolized into a compound that acts like a powerful full-agonist. However, at higher milligram doses, buprenorphine acts like the partial-agonist discussed in this piece. To put this into perspective, it helps to understand that buprenorphine is used in Europe to treat moderate to severe pain in the form of the butran patch. This patch is dosed at only 25 micrograms of buprenorphine that is slowly released over time. At these doses, in the non-buprenorphine dependent individual, a portion of the buprenorphine is metabolized into norbuprenorphine, a potent full-agonist like heroin or methadone that is thirty times the strength of morphine! However, at milligram doses used for addiction treatment, there is far too much buprenorphine, which, as discussed, has one of the highest affinities for the μ-opioid receptor, and beats out any norbuprenorphine that may be metabolized. Indeed, recreational drug users in online drug forums talk about the “less is more” phenomenon when it comes to Suboxone and buprenorphine pharmacology when referring to abusing buprenorphine for its recreational effects. Additionally, the movie “Reindeer Spotting” explores the epidemic of buprenorphine abuse in Finland, demonstrating the darker sides of this newer medication that is being used to combat the opioid epidemic. The fact that Suboxone and buprenorphine formulations are available by prescription and do not require daily dosing in a controlled clinic provides for greater illicit drug diversion than is possible with methadone.
Works Cited
- Maintenance Medication for Opiate Addiction: The Foundation of Recovery. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3411273/.
- Daniulaityte, R., Carlson, R., Brigham, G., Cameron, D. & Sheth, A. “Sub is a weird drug:” A Web-based study of lay attitudes about use of buprenorphine to self-treat opioid withdrawal symptoms. Am. J. Addict. Am. Acad. Psychiatr. Alcohol. Addict. 24, 403–409 (2015).
- Buprenorphine-based regimens and methadone for the medical management of opioid dependence: selecting the appropriate drug for treatment. – PubMed – NCBI. https://www.ncbi.nlm.nih.gov/pubmed/20958853.
- Buprenorphine vs methadone treatment: A review of evidence in both developed and developing worlds. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3271614/.
- Hämmig, R. et al. Use of microdoses for induction of buprenorphine treatment with overlapping full opioid agonist use: the Bernese method. Subst. Abuse Rehabil. 7, 99–105 (2016).
- Alford, D. P. et al. Collaborative care of opioid-addicted patients in primary care using buprenorphine: five-year experience. Arch. Intern. Med. 171, 425–431 (2011).
- Lofwall, M. R. & Havens, J. R. Inability to access buprenorphine treatment as a risk factor for using diverted buprenorphine. Drug Alcohol Depend. 126, 379–383 (2012).
- Long-acting opioid-agonists in the treatment of heroin addiction: why should we call them ‘substitution’? – PubMed – NCBI. https://www.ncbi.nlm.nih.gov/pubmed/19360539.
- Rosado, J., Walsh, S. L., Bigelow, G. E. & Strain, E. C. Sublingual Buprenorphine/Naloxone Precipitated Withdrawal in Subjects Maintained on 100 mg of Daily Methadone. Drug Alcohol Depend. 90, 261–269 (2007).
- Tompkins, D. A. et al. Concurrent Validation of the Clinical Opiate Withdrawal Scale (COWS) and Single-Item Indices against the Clinical Institute Narcotic Assessment (CINA) Opioid Withdrawal Instrument. Drug Alcohol Depend. 105, 154–159 (2009).
- Center for Substance Abuse Treatment. Clinical Guidelines for the Use of Buprenorphine in the Treatment of Opioid Addiction. (Substance Abuse and Mental Health Services Administration (US), 2004).
- Mendelson, J., Jones, R. T., Welm, S., Brown, J. & Batki, S. L. Buprenorphine and naloxone interactions in methadone maintenance patients. Biol. Psychiatry 41, 1095–1101 (1997).
- Suboxone Versus Methadone for the Detoxification of Patients Addicted to Prescription Opioids: A Review of Comparative Clinical Effectiveness, Safety, and Guidelines. 13.
- Johnson City Press: Suboxone: When a treatment becomes a problem. https://www.johnsoncitypress.com/Column/2019/05/05/Suboxone-When-a-treatment-becomes-a-problem.
- Naloxone‐induced withdrawal in patients with buprenorphine dependence – NIGAM – 1994 – Addiction – Wiley Online Library. https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1360-0443.1994.tb00898.x.
- Singh, R. A., Mattoo, S. K., Malhotra, A. & Varma, V. K. Cases of buprenorphine abuse in India. Acta Psychiatr. Scand. 86, 46–48 (1992).
- Harris, D. S. et al. Buprenorphine and naloxone co-administration in opiate-dependent patients stabilized on sublingual buprenorphine. Drug Alcohol Depend. 61, 85–94 (2000).
- The misuse of buprenorphine and a buprenorphine-naloxone combination in Wellington, New Zealand. – PubMed – NCBI. https://www.ncbi.nlm.nih.gov/pubmed/8370341.
- Bruce, R. D., Govindasamy, S., Sylla, L., Kamarulzaman, A. & Altice, F. L. Lack of Reduction in Buprenorphine Injection After Introduction of Co-Formulated Buprenorphine/Naloxone to the Malaysian Market. Am. J. Drug Alcohol Abuse 35, 68–72 (2009).
- Justice Department Obtains $1.4 Billion in Largest Opioid Drug Case Recovery in U.S. History | USPS Office of Inspector General. https://www.uspsoig.gov/document/justice-department-obtains-14-billion-largest-opioid-drug-case-recovery-us-history.
- Buprenorphine: A Unique Drug with Complex Pharmacology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2581407/.
Feature Image Credit: https://www.statnews.com/2019/03/12/deregulate-buprenophine-prescribing/