by Gaurav Dubey (MS Biotechnology)
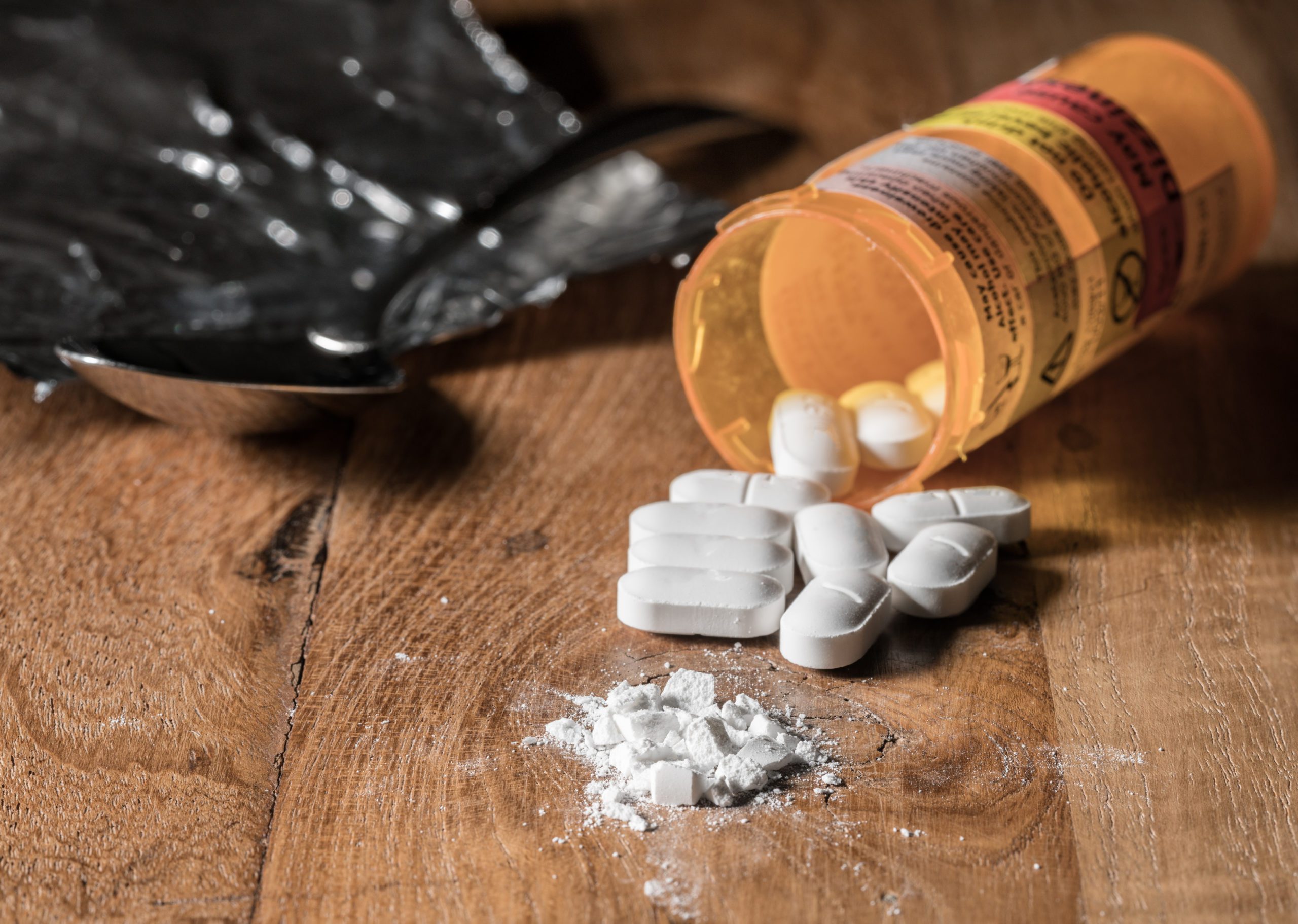
The evolution of pain management in medicine has been a remarkable one bringing significant controversy and contention. With over 100 million Americans suffering from chronic pain amidst the backdrop of the opioid epidemic, the need for non-narcotic and drug-free solutions to manage pain is greater than ever. This blog will explore the nature of chronic pain and describe five methods to manage chronic pain without the use of addictive medications, as per the latest clinical research.

Pain Without a Positive Purpose: Understanding the Nature of Chronic Pain
Pain is an “unpleasant sensory and emotional experience associated with actual or potential tissue damage, or [is] described in terms of such damage” even when there no such physical abnormalities exist.2,3 The primary purpose of pain is to help the organism experiencing pain to become aware of harmful events and “promote healing by causing sensitivity to movement or other stimuli that may delay recovery.”2 However, not all pain serves a useful, protective function, such as neuropathic pain, which may be the result of lesions or other neurological disorders.4 Persistent pain that does not serve the purpose to protect the body can be truly challenging to deal with—especially for those recovering from opioid use disorder and other addictions relating to their pain. Our current clinical understanding of pain is a complex subject to substantial variation across individuals.2 Patients suffering from chronic pain can benefit from exposure to a variety of supplemental, combination therapies that can help them manage their pain without the use of addictive drugs such as Vicodin, Oxycodone, and Xanax.

Chronic Pain is a Growing Public Health Concern—Especially for Recovering Addicts
Chronic pain is a growing public health concern and can seriously detract from an individual’s quality of life. A 2013 study by the Global Burden of Disease revealed chronic lower back pain was the “leading cause of years lived with disability.” Dealing with chronic pain in recovery can be especially challenging, particularly for those who were using opioids or other addictive substances, such as benzodiazepines, to manage their symptoms. The evidence is now clearer than ever that opioids should not be used to manage chronic pain and that there are very real dangers of abuse, dependence, and even overdose if used for prolonged periods of time to manage non-cancer-related chronic pain. For this reason, it is imperative for individuals in recovery to try and manage their pain without the use of dangerous and addictive substances.
The following lists five ways to manage chronic pain without the use of narcotic drugs that have been proven efficacious through rigorous scientific trials.
Acupuncture has been identified by the American College of Physicians for the treatment of chronic lower back pain, one of the most prevalent forms of chronic pain afflicting the world today. All three recommendations provided by physicians conducting the study strongly advised not to utilize opioids unless all other treatment options have failed. Acupuncture involves the strategic insertion of tiny needles into particular points in the body. A 1997 NIH panel found acupuncture to be effective for a variety of pain syndromes, including chemotherapy-induced pain and post-operative dental pain. Other conditions found to be effectively managed by acupuncture include fibromyalgia and osteoarthritis.
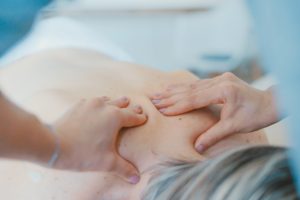
Massage has also been proven to be effective for the management of hard-to-control pain. “Massage is defined as pressing, rubbing, and manipulating the skin, muscles, tendons, and ligaments, with pressure ranging from light stroking to deep pressure”.9 Unlike the old days, massage therapy is no longer restricted to luxury spas and upscale health clubs. In fact, massage therapy can be found in offices, businesses and even airports in the modern day. Even more important is the fact that many health insurance plans cover massage therapy through chiropractic care–another great remedy for managing hard to treat pain without the use of drugs. The Mayo Clinic defines various types of massage, including Swedish massage, deep tissue massage, sports massage, and trigger point massage. 9 Besides aiding with chronic pain, here are some other benefits of massage therapy that can help individuals in recovery:
• Anxiety
• Depression
• Insomnia
• Headaches
• Stress
As with any therapy and medical intervention, it is important to consult with your physician before engaging in regular massage therapy. Seeking out the care of a well-trained professional is always strongly recommended, as is regular follow-up with one’s primary physician.
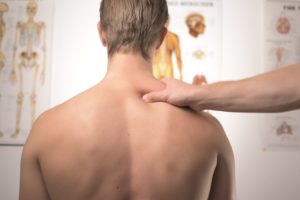
Chiropractic Care involves the utilization of various non-surgical treatments, such as spinal manipulation, to address symptoms of chronic pain.10 Most often, this entails the quick and deliberate application of pressure to the spine between two vertebrates. While the central focus of chiropractic care is spinal manipulation, chiropractors may also include other treatments, including manual or manipulative therapies, postural and exercise education, and ergonomic training (how to walk, sit, and stand to limit back strain).11 The American College of Physicians strongly recommends chiropractic care for the treatment of chronic lower back pain along with adding heat therapy, massage, and acupuncture.
Cognitive & Behavioral Therapy or CBT is a psychological treatment that has recently been shown to be an effective tool in managing chronic pain and improving the quality of life in patients who suffer from chronic pain. This treatment “involves practical techniques to change physical activity, reduce distress and catastrophizing, and improve functioning and social engagement.”2 Such techniques can include exposure to feared activities, the development of effective, non-pharmacologic coping strategies, and relaxation training. “The perception of pain is in your brain, so you can affect physical pain by addressing thoughts and behaviors that fuel it,” Hullett tells WebMD.12 While most chronic pain patients don’t want to be told “it’s all in your head,” CBT has shown to be a novel approach that may greatly improve one’s quality of life by helping to reduce pain levels.
Non-Narcotic Analgesic Drugs such as NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) can be incredibly effective in managing chronic pain and the side effects may be tolerable in some patients. This class of medication includes ibuprofen and is comprised of brand-name drugs such as Advil and Motrin. However, such compounds are well known to cause gastrointestinal, hematological, and kidney side effects—a significant problem for many patients.13 In such cases, other non-narcotic analgesics such as aspirin, aniline derivatives such as paracetamol (acetaminophen), and non-acidic pyrazole drugs like propyphenazone and dipyrone (metamizole).13 As with any medication, it is imperative for patients to seek the counsel of their primary care physician or board-certified medical professional. This blog, while intended to be informative, is not intended to take the place of professional medical advice.
Chronic Pain Can Be Difficult To Manage In Sobriety, But Not Impossible
Managing chronic pain in recovery can undoubtedly be challenging, but if patients are diligent about trying the aforementioned techniques, this author and biologist in recovery certainly believe it is possible. In my personal journey through recovery, managing significant chronic pain from pelvic floor dysfunction to irritable bowel syndrome has been difficult, but not impossible. Techniques such as acupuncture and CBT certainly require a degree of patience, faith, and willingness, but so does recovery! The brain is a powerful instrument and can either work for us or against us. By harnessing the above treatment and therapies, one can truly maximize their chances of success in recovery by avoiding the use of addicting opioids and other narcotic drugs. If you or a loved one is struggling with substance abuse, visit EvolveIndy.com